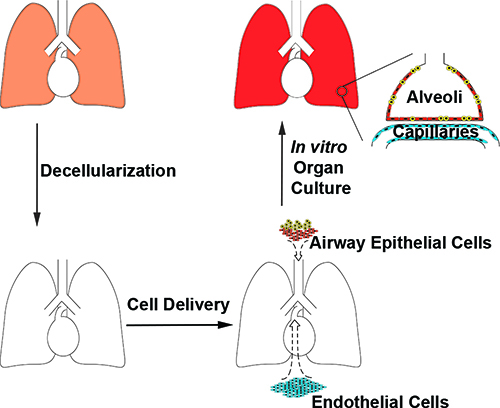
Bioengineered lungs
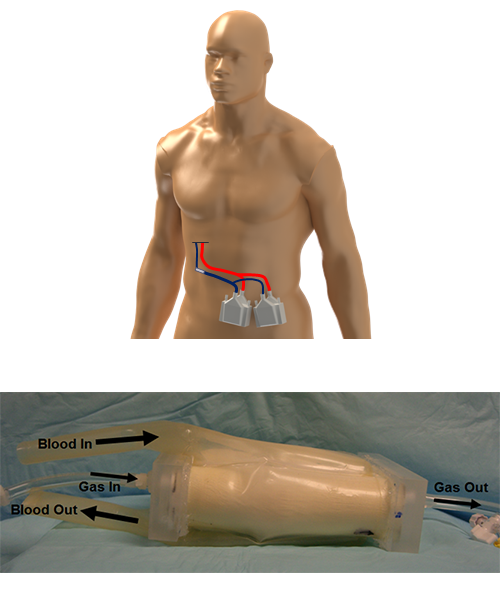
Carnegie Mellon researchers are developing new devices and technologies to create a permanent solution to chronic lung disease. The team is focused on changing the way patients will one day be able to receive respiratory support: years of support in the comfort of their own home.
Bioengineered lungs
Explore Other Research Topics