Cook Cardiopulmonary Engineering Group
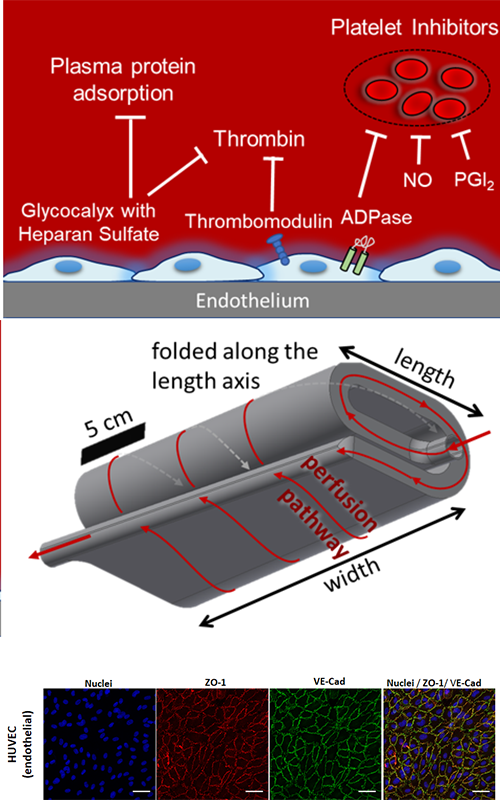
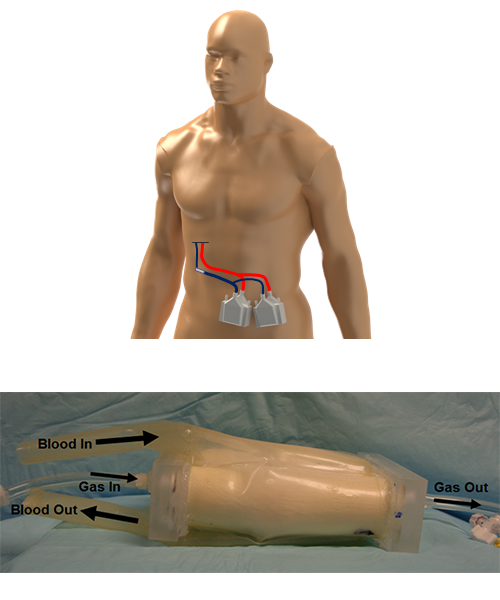
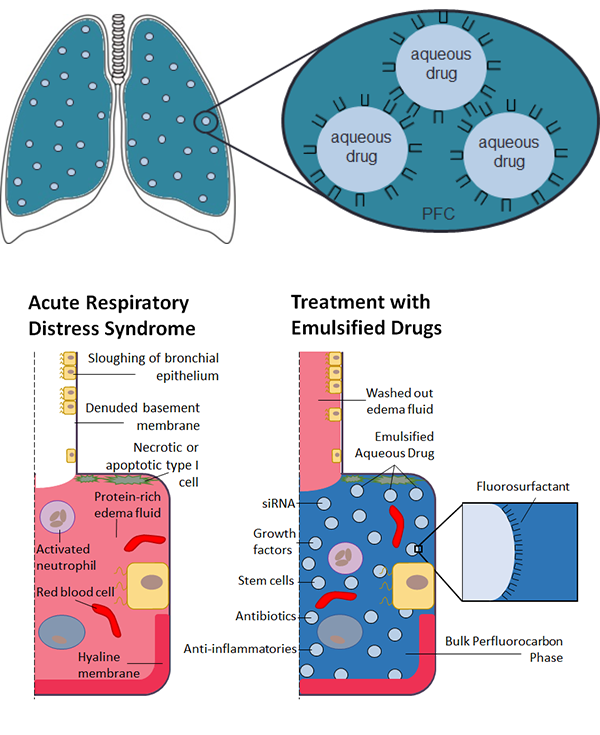
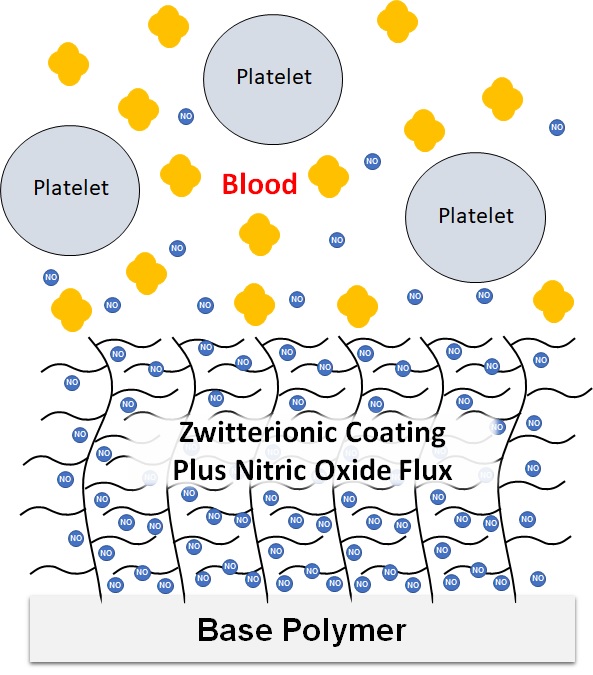
Keith Cook’s research focuses on applying engineering to critical care medicine. This research melds mechanical, chemical, and material science concepts toward the development of artificial and tissue-based lungs, pulmonary drug delivery, and the computational modeling and prevention of coagulation in medical devices.